Connect With Us
Blog
Blog
Symptoms of Gout
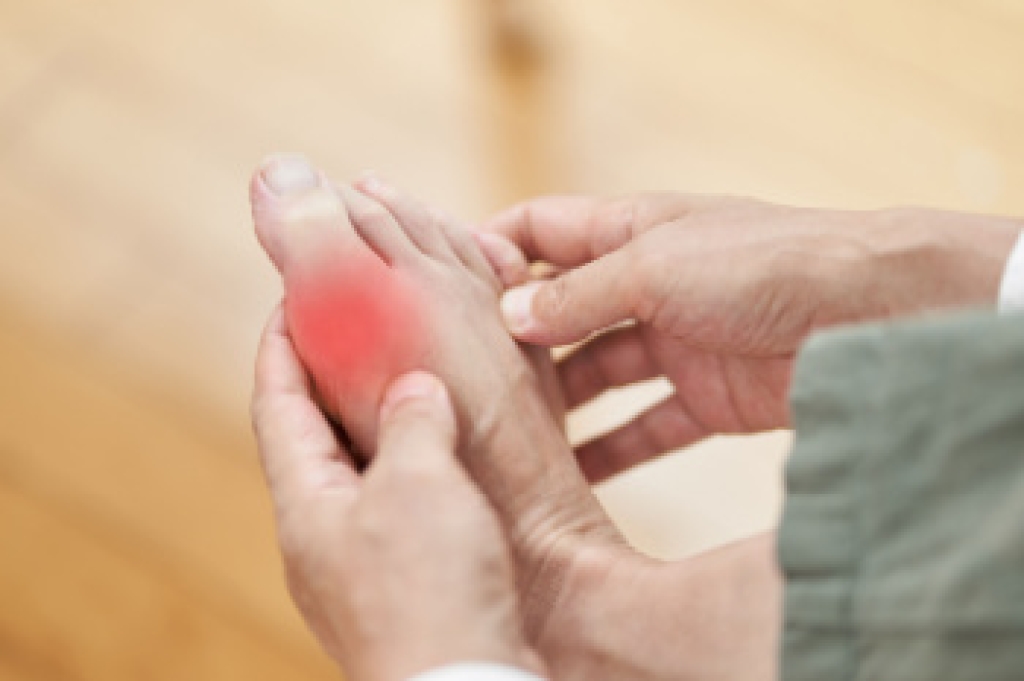
Gout is a form of arthritis that can cause sudden episodes of severe pain in the feet and ankles when uric acid crystals collect inside a joint. Gout frequently affects the big toe, but it may also involve the arch, heel, or ankle. During a flare-up, the joint may become swollen, stiff, and extremely sensitive. Skin often appears red or purple and feels warm to the touch. Some patients describe the pain as sharp, crushing, or pulsating, making it difficult to walk or wear shoes comfortably. Gout attacks may be the result of dehydration, alcohol use, certain medications, or diets high in purine-rich foods. Repeated inflammation can damage cartilage and surrounding tissue. A podiatrist can examine the painful area, evaluate joint changes, and help guide treatment to reduce inflammation and prevent future attacks. Care may include medication recommendations, footwear guidance, and strategies to reduce pressure on the affected joints. If you have symptoms of gout, it is suggested that you schedule an appointment with a podiatrist for relief and prevention tips from this painful condition.
Gout is a painful condition that can be treated. If you are seeking treatment, contact one of our podiatrists from East Ocean Podiatry . Our doctors will treat your foot and ankle needs.
What Is Gout?
Gout is a form of arthritis that is characterized by sudden, severe attacks of pain, redness, and tenderness in the joints. The condition usually affects the joint at the base of the big toe. A gout attack can occur at any random time, such as the middle of the night while you are asleep.
Symptoms
- Intense Joint Pain - Usually around the large joint of your big toe, and it most severe within the first four to twelve hours
- Lingering Discomfort - Joint discomfort may last from a few days to a few weeks
- Inflammation and Redness -Affected joints may become swollen, tender, warm and red
- Limited Range of Motion - May experience a decrease in joint mobility
Risk Factors
- Genetics - If family members have gout, you’re more likely to have it
- Medications - Diuretic medications can raise uric acid levels
- Gender/Age - Gout is more common in men until the age of 60. It is believed that estrogen protects women until that point
- Diet - Eating red meat and shellfish increases your risk
- Alcohol - Having more than two alcoholic drinks per day increases your risk
- Obesity - Obese people are at a higher risk for gout
Prior to visiting your podiatrist to receive treatment for gout, there are a few things you should do beforehand. If you have gout you should write down your symptoms--including when they started and how often you experience them, important medical information you may have, and any questions you may have. Writing down these three things will help your podiatrist in assessing your specific situation so that he or she may provide the best route of treatment for you.
If you have any questions, please feel free to contact our office located in Deerfield Beach, FL . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Lingering Ankle Pain
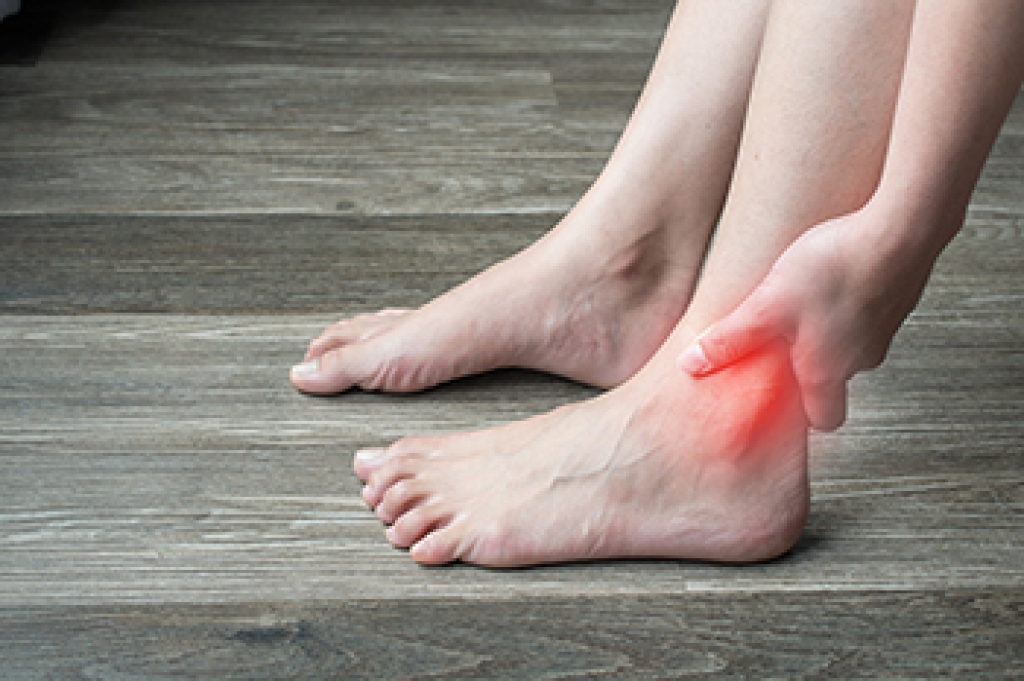
Ankle impingement syndrome develops when soft tissue or bone in the ankle becomes compressed during movement, often after repeated sprains or ongoing instability. Many people notice pain at the front or back of the ankle, especially while walking uphill, squatting, running, or pointing the foot downward. Swelling, stiffness, and a limited range of motion are also common. In some cases, scar tissue or bony growths form inside the joint and create ongoing irritation each time the ankle bends. Athletes and active individuals are frequently affected, but anyone with a history of ankle injuries can develop this condition. A podiatrist can evaluate joint movement, order imaging studies, identify areas of inflammation, and recommend treatments designed to reduce pressure within the ankle. Care may include bracing, custom orthotics, targeted exercises, anti-inflammatory treatment, or surgical correction when symptoms become severe. It is strongly suggested that people with chronic ankle pain or restricted motion visit a podiatrist for an evaluation and appropriate care.
Ankle pain can have many different causes and the pain may potentially be serious. If you have ankle pain, consult with one of our podiatrists from East Ocean Podiatry . Our doctors will assess your condition and provide you with quality foot and ankle treatment.
Ankle pain is any condition that causes pain in the ankle. Due to the fact that the ankle consists of tendons, muscles, bones, and ligaments, ankle pain can come from a number of different conditions.
Causes
The most common causes of ankle pain include:
- Types of arthritis (rheumatoid, osteoarthritis, and gout)
- Ankle sprains
- Broken ankles
- Achilles tendinitis
- Achilles tendon rupture
- Stress fractures
- Tarsal tunnel syndrome
- Plantar fasciitis
Symptoms
Symptoms of ankle injury vary based upon the condition. Pain may include general pain and discomfort, swelling, aching, redness, bruising, burning or stabbing sensations, and/or loss of sensation.
Diagnosis
Due to the wide variety of potential causes of ankle pain, podiatrists will utilize a number of different methods to properly diagnose ankle pain. This can include asking for personal and family medical histories and of any recent injuries. Further diagnosis may include sensation tests, a physical examination, and potentially x-rays or other imaging tests.
Treatment
Just as the range of causes varies widely, so do treatments. Some more common treatments are rest, ice packs, keeping pressure off the foot, orthotics and braces, medication for inflammation and pain, and surgery.
If you have any questions please feel free to contact our office located in Deerfield Beach, FL . We offer the newest diagnostic tools and technology to treat your foot and ankle needs.
Facts About Detached Toenails
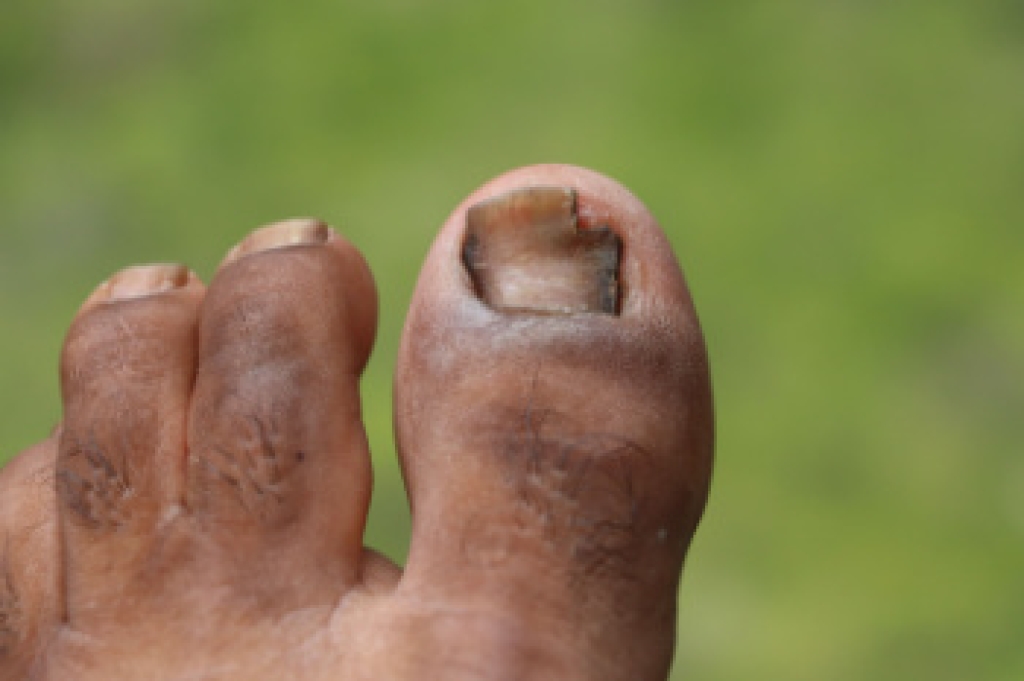
A detached toenail can occur from direct injury, fungal infections, psoriasis, or complications related to diabetes. Once a toenail separates from the nail bed, it cannot be reattached and must be allowed to grow out naturally as a new nail forms. Risk factors include repetitive trauma, wearing tight footwear, poor circulation, and underlying skin or metabolic conditions. Symptoms include pain, discoloration, thickening, or complete nail lifting. A podiatrist can evaluate the cause, safely manage the affected nail, help prevent infection, and support healthy regrowth with proper care. They can also help address underlying conditions that contribute to nail problems. If your toenail has fallen off, it is suggested that you consult a podiatrist who can determine the cause and guide you toward management tips as the new nail grows in.
Toe pain can disrupt your daily activities. If you have any concerns, contact one of our podiatrists of East Ocean Podiatry . Our doctors can provide the care you need to keep you pain-free and on your feet.
What Causes Toe Pain?
Most severe toe pain is caused due to a sports injury, trauma from dropping something heavy on the toe, or bumping into something rigid. Other problems can develop over time for various reasons.
Toe pain can be caused by one or more ailments. The most common include:
- Trauma
- Sports injury
- Wearing shoes that are too tight
- Arthritis
- Gout
- Corns and calluses
- Hammertoe
- Bunions
- Blisters
- Ingrown toenails
- Sprains
- Fractures (broken bones)
- Dislocations
When to See a Podiatrist
- Severe pain
- Persistent pain that lasts more than a week
- Signs of infection
- Continued swelling
- Pain that prevents walking
Diagnosis
In many cases the cause of toe pain is obvious, but in others, a podiatrist may want to use more advanced methods to determine the problem. These can range from simple visual inspections and sensation tests to X-rays and MRI scans. Prior medical history, family medical history, and any recent physical traumatic events will all be taken into consideration for a proper diagnosis.
Treatment
Treatments for toe pain and injuries vary and may include shoe inserts, padding, taping, medicines, injections, and in some cases, surgery. If you believe that you have broken a toe, please see a podiatrist as soon as possible.
If you have any questions please contact our office located in Deerfield Beach, FL . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Understanding Foot and Ankle Pain From Bicycling

Foot and ankle pain while cycling is often related to bike setup and support. Achilles tendonitis can develop from the pedaling motion, especially when the saddle is set too high. This can lead to tightness and pain in the back of the ankle. Ankle discomfort may also occur in those with flat feet, which can affect stability during each pedal stroke. Foot pain is often linked to wearing shoes that lack proper support or riding in too high a gear. These factors increase pressure against the pedal and cause soreness or burning pain. Risk factors include repetitive motion, poor alignment, and improper equipment. A podiatrist can evaluate your foot mechanics and recommend supportive solutions. If cycling pain is limiting your rides, it is suggested that you consult a podiatrist who can provide effective relief solutions, enabling you to return to this popular activity.
Sports related foot and ankle injuries require proper treatment before players can go back to their regular routines. For more information, contact one of our podiatrists of East Ocean Podiatry . Our doctors can provide the care you need to keep you pain-free and on your feet.
Sports Related Foot and Ankle Injuries
Foot and ankle injuries are a common occurrence when it comes to athletes of any sport. While many athletes dismiss the initial aches and pains, the truth is that ignoring potential foot and ankle injuries can lead to serious problems. As athletes continue to place pressure and strain the area further, a mild injury can turn into something as serious as a rupture and may lead to a permanent disability. There are many factors that contribute to sports related foot and ankle injuries, which include failure to warm up properly, not providing support or wearing bad footwear. Common injuries and conditions athletes face, including:
- Plantar Fasciitis
- Achilles Tendinitis
- Achilles Tendon Rupture
- Ankle Sprains
Sports related injuries are commonly treated using the RICE method. This includes rest, applying ice to the injured area, compression and elevating the ankle. More serious sprains and injuries may require surgery, which could include arthroscopic and reconstructive surgery. Rehabilitation and therapy may also be required in order to get any recovering athlete to become fully functional again. Any unusual aches and pains an athlete sustains must be evaluated by a licensed, reputable medical professional.
If you have any questions please contact our office located in Deerfield Beach, FL . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Blog Archives
- 2026
- 2025
- 2024
- 2023
- 2022

